Standardized Patient
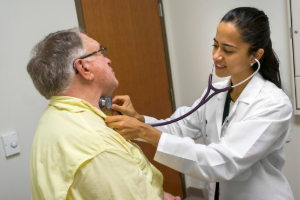 A standardized patient or SP is an individual trained to portray a
specific patient case in a consistent manner. SPs learn to appear as the
patient by using specific body language, movement and responses to
physical examination. During an interaction
with a medical student, the SP presents the case history in response
to questioning by the student and/or undergoes physical examinations at
the student's direction. Each SP encounter is designed to assess a
student's communication and/or physical
examination skills. These encounters allow students the opportunity
to develop, practice and enhance their medical interviewing skills,
communication skills and physical exam techniques. The opportunity to
practice on real people and receive feedback
on how it feels to be their patient is an experience students only
get in this simulated setting making SP work crucial to medical
education and impactful for future generations patients.
A standardized patient or SP is an individual trained to portray a
specific patient case in a consistent manner. SPs learn to appear as the
patient by using specific body language, movement and responses to
physical examination. During an interaction
with a medical student, the SP presents the case history in response
to questioning by the student and/or undergoes physical examinations at
the student's direction. Each SP encounter is designed to assess a
student's communication and/or physical
examination skills. These encounters allow students the opportunity
to develop, practice and enhance their medical interviewing skills,
communication skills and physical exam techniques. The opportunity to
practice on real people and receive feedback
on how it feels to be their patient is an experience students only
get in this simulated setting making SP work crucial to medical
education and impactful for future generations patients.
Do the medical students know SPs are not real patients?
Yes, the students are aware that SPs are not real patients. They work in collaboration with the standardized patients to achieve their goals. Receiving feedback from their SPs from the patient perspective is unique to simulation. This relationship gives students first-hand insight into how they will approach their own medical practices in future clinical settings.
How do SPs know what to say when the medical student interviews them?
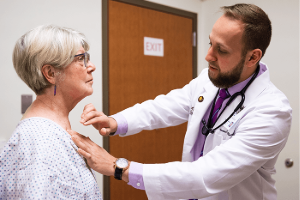 SPs
are carefully trained to portray a specific patient. They learn the
complete medical history of the patient and tell the students details
about their lives, such as work, family and hobbies. SPs are trained to
depict the patient's appropriate emotional
state as well. It may be appropriate to appear anxious, irritable or confused during an interview, if that is part of the scenario. For
cases requiring a physical exam, SPs know how to move as the patient
would and simulate findings while being examined.
In addition to portraying the case, it is important to observe the
behavior of the learners to provide balanced and objective feedback
allowing the students to reflect on the session when receiving feedback
from the patient point of view.
SPs
are carefully trained to portray a specific patient. They learn the
complete medical history of the patient and tell the students details
about their lives, such as work, family and hobbies. SPs are trained to
depict the patient's appropriate emotional
state as well. It may be appropriate to appear anxious, irritable or confused during an interview, if that is part of the scenario. For
cases requiring a physical exam, SPs know how to move as the patient
would and simulate findings while being examined.
In addition to portraying the case, it is important to observe the
behavior of the learners to provide balanced and objective feedback
allowing the students to reflect on the session when receiving feedback
from the patient point of view.
What type of physical examinations are performed?
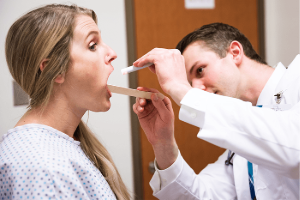 If the
students are expected to perform physical examinations, SPs may be
required to wear hospital gowns. Students perform focused physical
examinations based on the patient's case. These examinations may include
listening to the heart and lungs with
a stethoscope, pressing on the abdomen, neck, face and limbs, using a
scope to look in the ears, eyes, nose and throat, taking a pulse or
blood pressure and checking muscle strength, reflexes, range of motion
and gait. The cases that require these
physical examinations are clearly outlined for the SPs prior to
their agreement to participate in them. For patient cases requiring no
physical examinations, SPs wear street clothes.
If the
students are expected to perform physical examinations, SPs may be
required to wear hospital gowns. Students perform focused physical
examinations based on the patient's case. These examinations may include
listening to the heart and lungs with
a stethoscope, pressing on the abdomen, neck, face and limbs, using a
scope to look in the ears, eyes, nose and throat, taking a pulse or
blood pressure and checking muscle strength, reflexes, range of motion
and gait. The cases that require these
physical examinations are clearly outlined for the SPs prior to
their agreement to participate in them. For patient cases requiring no
physical examinations, SPs wear street clothes.
Is it safe?
Yes. The examinations are very basic and are harmless to the patient. No real injection or invasive techniques are performed on the SPs. All encounters are videotaped, and most interactions are observed as they happen, in part for the safety and comfort of the SP.
Do SPs have to grade the students?
Part of the SP job is to record the events of the encounters on a checklist to score the student. SPs are trained to either write feedback or lead a conversation with the student. This feedback helps the student reflect on their communication skills with a focus on the perspective of the patient. Faculty members ultimately decide how students are scored for exercises.
Do SPs need to know a lot about medicine?
No. Standardized patient cases contain all the information one needs for portrayal and
feedback and with the training sessions beforehand, SPs are ready to
interact with the students as the cases require.
How often do SPs work?
The work can be temporary, part-time and seasonal. SP sessions are scheduled according to student needs and program requirements. SPs with greater ranges of availability and willingness to work in multiple locations will have the opportunity for more sessions.
What else is important to becoming a standardized patient?
It is important to maintain the patient's character and physical condition during an encounter. This job entails good concentration while being interviewed and examined to recall techniques for physical exam checklists and communication skills for feedback. At times, SPs may also provide verbal feedback directly to the students. Great SPs are reliable, good communicators, focused, have good memories and are comfortable with their own bodies.
What is the hiring process?
 After receiving the
applications, the SP team will reach out to schedule phone interviews
with viable candidates. From there, selected candidates will be invited
in for an interactive interview where they will get the opportunity to
portray a patient,
fill out a checklist and provide feedback. This format allows the SP
team to assess the candidate and provides the opportunity for the
applicant to experience the role of the SP. Characteristics looked for
in the interview are a positive attitude,
no biases toward gender, race, religion, national origin, or
physical characteristics, reliability and punctuality, an understanding
of confidential matters, a willingness to adapt to new technology,
timeliness of communication through email and the
ability to be comfortable with one's own health.
After receiving the
applications, the SP team will reach out to schedule phone interviews
with viable candidates. From there, selected candidates will be invited
in for an interactive interview where they will get the opportunity to
portray a patient,
fill out a checklist and provide feedback. This format allows the SP
team to assess the candidate and provides the opportunity for the
applicant to experience the role of the SP. Characteristics looked for
in the interview are a positive attitude,
no biases toward gender, race, religion, national origin, or
physical characteristics, reliability and punctuality, an understanding
of confidential matters, a willingness to adapt to new technology,
timeliness of communication through email and the
ability to be comfortable with one's own health.
Gynecological and male urogenital teaching associate
What is a GTA?
Gynecological teaching associates (GTAs) are women who are specifically trained to teach the sensitive exam, and assess and provide feedback to learners about accurate pelvic and/or breast examination techniques. GTAs use their bodies to guide students through the entire process of performing a thorough pelvic exam: a visual exam (checking for any lumps or bumps), a speculum exam and a bi-manual exam. The GTAs coach medical students on their clinical skills and give hands-on instruction, as well as comments on technique, language and overall approach. They also address the communication skills needed to provide a comfortable exam in a standardized manner while using their bodies as teaching tools in a supportive, non-threatening environment.
What is a MUTA?
Male urogenital teaching associates (MUTAs) are men who are specially trained to teach, assess and provide feedback to learners about accurate urogenital and rectal examination techniques. A MUTA will address the communication skills needed to provide comfortable exams in a standardized manner while using their bodies as teaching tools in a supportive, non-threatening environment. MUTAs teach the proper technique for performing the urogenital exam, including external and internal inspection and palpation. Urological exam procedures include palpation for lymph nodes, hernias, and examination of the scrotum, testicles, penis, and rectum (prostate) and breast. MUTAs will guide the student through the learning process while each learner performs the urologic exam on the MUTA's body.
We are recruiting people who are interested in contributing their talents to further medical education and influence patient outcomes in the future.
There are also those who regard GTA and MUTA work as a form of activism, promoting sex-positive health care. They will become confident and certified through our intensive training session. As always at the Covenant HealthCare College of Medicine, professionalism and dependability are also essential. GTAs and MUTAs provide a unique opportunity to be involved in shaping the medical education of tomorrow's physicians and health professionals.
Next steps
Using the buttons below, please fill out the appropriate application to be considered for a position. Please note that a resume is required and a cover letter is suggested.